Spider veins are a common cosmetic and sometimes uncomfortable vascular concern that affects millions of people, particularly busy professionals who spend long hours standing, sitting, or traveling. A spider vein removal in Tucson provides targeted, specialist-led care that addresses both appearance and underlying venous health. A qualified vein doctor evaluates symptoms, identifies the root causes, and offers treatments—from sclerotherapy to energy-based procedures—that minimize downtime while improving circulation and comfort. This article explains what spider veins are, how they are diagnosed, the treatment options available, what to expect during recovery, and practical strategies for prevention, giving online business owners, agency leaders, and marketers concise, evidence-based guidance to make informed decisions quickly.
What are Spider Veins and Who Gets Them
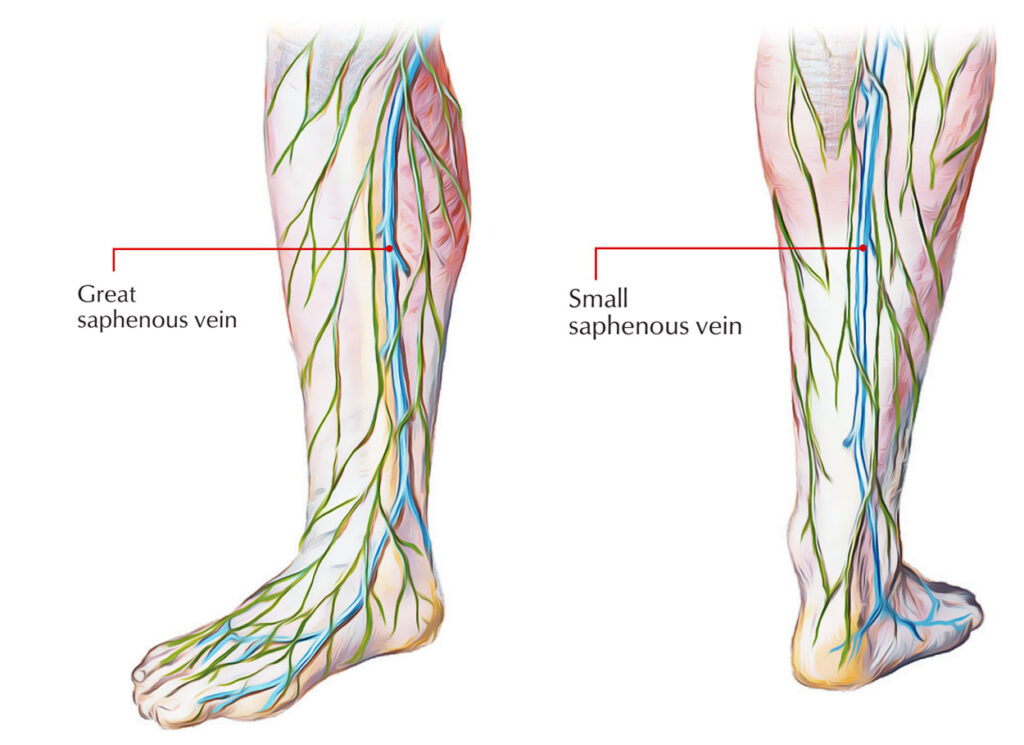
Spider veins, medically called telangiectasias, are small dilated blood vessels visible near the skin’s surface, commonly on the legs and face. They appear as thin red, blue, or purple lines that branch like a spider’s web. Unlike varicose veins, which are larger and bulging, spider veins are typically flat and cosmetic, though they may accompany discomfort.
Common Causes and Risk Factors
A specialist will note that spider veins result from increased pressure in superficial veins and weakness in venous walls. Typical risk factors include:
- Genetics: A family history of venous disease strongly raises the likelihood.
- Age and Hormones: Incidence rises with age: hormonal shifts in pregnancy, puberty, and menopause contribute.
- Gender: Women are more frequently affected, partly due to pregnancies and hormonal therapies.
- Prolonged Standing or Sitting: Occupations that require long periods on the feet or seated reduce calf-muscle pump efficiency.
- Obesity and Sedentary Lifestyle: Both increase venous pressure.
- Prior Leg Injury or Thrombosis: Damage or past blood clots can alter normal venous flow.
Understanding causes helps prioritize treatment: if superficial spider veins stem from deeper venous reflux, a specialist will address the underlying problem first.
Symptoms, When to Seek Specialist Care, and Red Flags
Many people seek treatment for cosmetic reasons, but symptoms can include aching, burning, itching, and nocturnal cramping. Seek specialist care if there’s:
- Persistent leg pain or swelling that doesn’t improve with conservative measures.
- Skin changes: discoloration, thickening, or ulceration near the ankle.
- Bleeding from a vein after minor trauma.
- Rapid enlargement of veins or new, unexplained symptoms.
These red flags may indicate chronic venous insufficiency or complications that need prompt evaluation and possibly more than cosmetic care.
How Specialists Diagnose Spider Veins
A careful diagnosis differentiates isolated cosmetic spider veins from disease that requires definitive venous intervention.
Physical Exam and Medical History
A vascular specialist begins with a focused history: symptom timeline, family history, pregnancies, prior deep vein thrombosis, and occupational habits. The physical exam inspects the legs standing and supine, assesses the distribution of spider veins, looks for varicose veins, skin changes, and evaluates the patient’s gait and calf muscle function. Simple bedside maneuvers (Trendelenburg or manual compression tests) give clues about venous valve competence.
Treatment Options Explained by a Specialist
Specialists tailor treatment to the patient’s anatomy, symptoms, and goals. Options range from conservative measures to minimally invasive procedures and, rarely, open surgery.
Minimally Invasive Procedures: Sclerotherapy, Laser, and RFA
- Sclerotherapy: The workhorse for spider veins on the legs and many facial vessels. A sclerosing solution (foam or liquid) is injected into targeted veins, irritating the vessel wall and causing it to collapse and fade over weeks. It’s office-based, has minimal downtime, and yields excellent cosmetic results when performed by an experienced clinician.
- Endovenous Laser Ablation (EVLA) and Radiofrequency Ablation (RFA): These heat-based therapies treat larger incompetent saphenous veins that often feed surface spider veins. By closing the refluxing source vein, specialists prevent the recurrence of new surface vessels. EVLA and RFA are performed under local anesthesia and ultrasound guidance.
- Surface Laser Therapies: For facial spider veins and small leg vessels not suitable for injection, pulsed dye lasers or intense pulsed light (IPL) devices target hemoglobin within vessels, causing selective photothermolysis. Results vary by skin type and vessel depth: multiple treatments may be needed.
Surgical and Office Procedures: Phlebectomy and Ablation
- Ambulatory Phlebectomy: For visible varicose tributaries, tiny incisions allow the removal of targeted veins under local anesthesia. It’s highly effective for discrete bulging veins and is often combined with ablation of the primary saphenous vein.
- Hybrid Approaches: Modern venous care often blends ablation of the source veins with phlebectomy and sclerotherapy for the best cosmetic and symptomatic outcomes.
Conservative Measures: Compression, Topicals, and Lifestyle Changes
Not every case requires a procedure. Conservative management includes graduated compression stockings, leg elevation, regular walking to activate the calf pump, weight management, and avoidance of prolonged immobility. Topical agents or over-the-counter creams may ease mild symptoms but won’t eliminate visible veins. Specialists use conservative therapy as primary care in mild cases or adjunctive post-procedure care.
What to Expect During Treatment: Preparation, Procedure, and Recovery
Knowing the practical steps reduces anxiety and helps patients plan recovery around busy schedules.
Typical Procedure Day and Immediate Aftercare
Most treatments are outpatient and can be done in a clinic room or an ambulatory center. Preparation typically involves:
- Pre-procedure consent and review of medications (blood thinners may need temporary adjustment).
- Marking veins while the patient stands to ensure accurate targeting.
- Local anesthesia for phlebectomy or ablation; sclerotherapy and surface laser usually require little or no anesthesia.
Immediately after sclerotherapy or ablation, compression bandages or stockings are applied. Patients are encouraged to walk shortly after treatment to reduce clot risk and improve outcomes. Mild bruising, redness, and tenderness are common and usually resolve within days to weeks.
Recovery Timeline, Side Effects, and Follow-Up Visits
Recovery is typically rapid: many return to desk work the same day and resume most activities within 48–72 hours. Expected post-procedure effects include bruising, temporary hyperpigmentation, and mild tightness. Rare but important complications include superficial thrombophlebitis, matting (new fine vessel formation), and, very rarely, deep vein thrombosis. Follow-up with ultrasound may be scheduled four to twelve weeks after treatment to confirm vein closure and guide additional care. Specialists often plan staged treatments months apart to optimize cosmetic results.
Choosing the Right Specialist and Questions to Ask
Selecting a qualified specialist ensures safety and predictable results.
Credentials, Experience, and Treatment Philosophy to Look For
Patients should seek vascular surgeons, interventional radiologists, or phlebologists with focused training in venous disease. Important indicators include:
- Board certification in vascular surgery, interventional radiology, or comparable fields.
- Procedural volume and before/after portfolios.
- Use of duplex ultrasound during evaluation and treatment planning.
- A conservative, evidence-based philosophy that treats underlying reflux rather than only cosmetic veins.
Ask about the clinician’s complication rates, technologies used, and whether they’ll provide a personalized plan that balances symptom relief, appearance goals, and long-term prevention.
Costs, Insurance Considerations, and Financing Options
Insurance may cover treatment when spider veins are symptomatic or tied to venous insufficiency: cosmetic-only procedures are usually out-of-pocket. A clear pre-treatment estimate should outline fees for consultation, procedures, imaging, and follow-up. Many practices offer financing or payment plans. Busy professionals should ask about scheduling flexibility and how many visits are likely: a streamlined process saves time and produces better adherence to follow-up care.
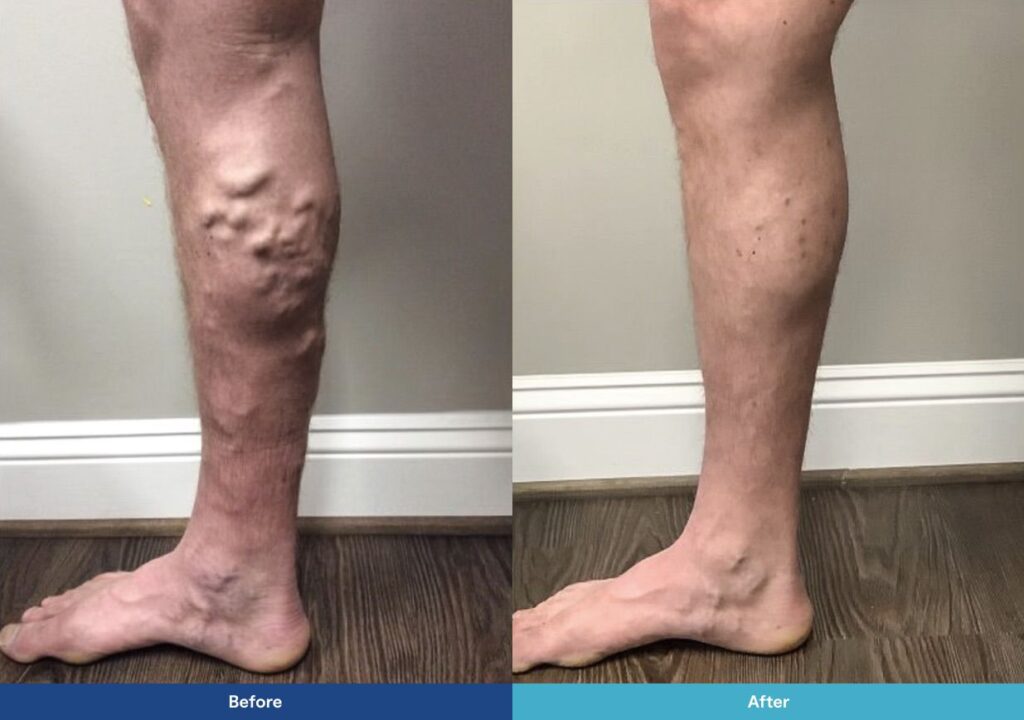
Preventing New Spider Veins and Maintaining Results
Maintenance combines practical habits and occasional touch-ups.
Lifestyle Habits, Compression Strategies, and When to Repeat Treatment
- Regular Movement: Walking daily for 30 minutes activates the calf pump and reduces venous pressure.
- Compression Stockings: Graduated stockings worn during prolonged standing or travel help prevent new vein formation and support recovery after procedures.
- Weight Management: Even modest weight loss reduces venous load.
- Avoid Prolonged Immobility: Break up extended periods of sitting with short walks or leg exercises.
Even with ideal habits, genetics and aging mean new spider veins can appear. Specialists often recommend periodic maintenance, sclerotherapy, or laser touch-ups every few years for cosmetic upkeep. Early intervention when new veins first appear typically yields simpler, faster treatments.
Conclusion
Spider veins are a treatable condition with a spectrum of options ranging from conservative measures to advanced, minimally invasive procedures. A specialist evaluates whether surface veins are a cosmetic issue or a sign of deeper venous disease and builds a staged plan that addresses both appearance and function. For busy professionals seeking efficient care, the right clinic combines evidence-based protocols, clear scheduling, and transparent cost estimates. When in doubt, an initial duplex-based assessment is the most valuable step; it clarifies the cause, streamlines treatment, and helps protect long-term results. Just as online businesses partner with specialized agencies for targeted growth, patients achieve the best vascular outcomes by working with specialists who match their needs, goals, and schedule.